Article at a glance
Conditions that involve the bones and joints can be a major burden on both individuals and healthcare systems.
Bone and joint conditions can often be overlooked, despite causing permanent disability in many people.
Bones weaken as you grow older, which can increase your risk of having fractures.
Fractures can be prevented through proper bone health screening.
Similar to bones, joints can deteriorate as you age, and this can lead to many different types of health issues.
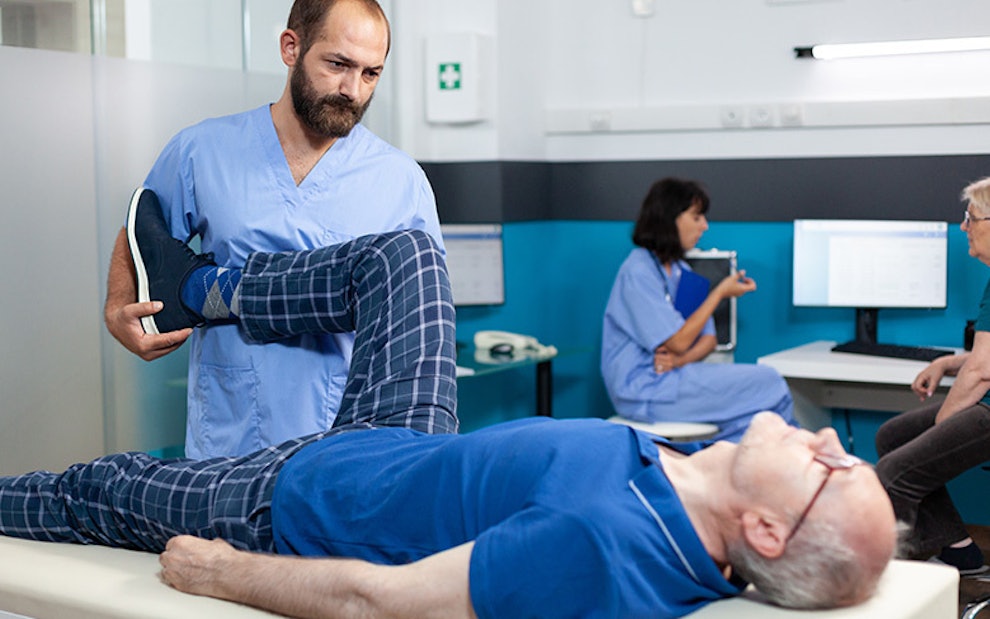
Why is it important to have healthy bones and joints?
Bone health
Bones serve as the structural framework of the body. They play a role in the body’s shape, strength, and support, and offer protection to certain organs like the brain, heart, and lungs. Bones serve as storage sites for certain minerals such as calcium and phosphorus, and they also house the bone marrow, which is where blood cells are developed and stored.
Bones weaken as you grow older, which increases your risk of osteoporosis. Osteoporosis happens when your bones lose their structural integrity to the point where they can break easily, resulting in fractures. Bones that are most affected include your hips, spine, and wrists. However, this weakening doesn’t happen overnight. In fact, osteoporosis is considered a “silent disease” because you don’t tend to notice that your bones have been losing strength over the course of many years.
Bones stay strong by replacing old bones with new ones. At around 30 years old, bones stops growing, and your bones are in a balanced state of breaking and building more bone. But by 40–50 years old, this balance shifts to where your bones are being broken down more than they’re being replaced. Osteoporosis can happen at any age and in either gender, but older adults and women tend to be more at risk. Other risk factors include:
being of White or Asian race
family history of fractures or osteoporosis
personal history of a fracture before 50 years old
early menopause
having ovaries surgically removed before menopause
lack of calcium or vitamin D
smoking
certain medications
small body frame
Although women lose bone mass quickly at the time of menopause, men and women lose bone at an equal rate by 65–70 years old.
There’s a similar disease called osteopenia (low bone mass), which is essentially a milder form of osteoporosis. If you’ve been diagnosed with osteopenia, take it as a warning sign and make the necessary steps to keep your bones strong and reduce your risk of progressing to osteoporosis. Osteoporosis is a common cause of fractures, which can cause severe pain. But depending on the severity, they can be debilitating as well, and even lead to death. Hospitalizations for fractures due to osteoporosis total more than that of heart attacks, strokes, and breast cancer combined. This highlights the importance of timely bone health screening, and subsequent preventative measures and interventions.
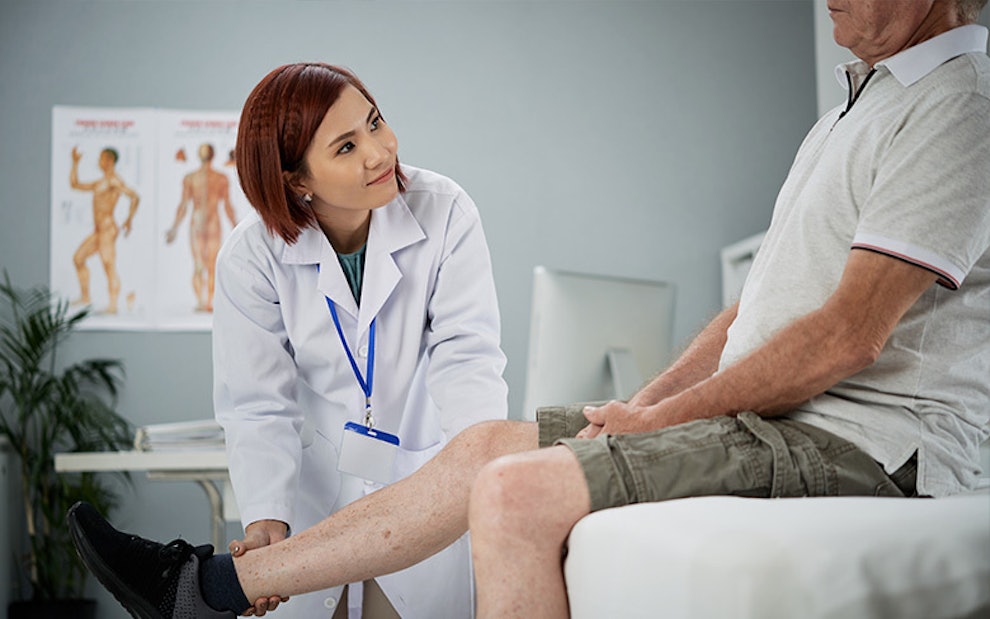
Joint health
A joint is the area where two bones meet. Similar to bones, joints play a role in supporting the body. There are two ways to classify joints: by composition or by function. Compositionally, joints can be divided into fibrous, cartilaginous, and synovial. Functionally, they can be immovable (synarthrosis), slightly movable (amphiarthrosis), or freely movable (diarthrosis).
Fibrous joints are fixed areas that can be found in sites where collagen connects bones. Examples include the bones that make up the skull, the area where the teeth are attached to the sockets, and the connection between the bones of the upper limbs (forearm and upper arm) and lower limbs (thigh and leg).
Cartilaginous joints can be found in areas where the bones are attached by cartilage. These include the pubic symphysis (area where the left and right pubic bones meet), intervertebral discs (area between the vertebral bones), and between the tip (epiphysis) and shaft (diaphysis) of growing long bones.
Synovial joints are freely movable, main functional joints of the body. They prevent friction between bones and permit varying degrees of mobility. They can be found in elbows, knees, ankles, hands, feet, shoulders, and hips.
Many diseases can affect the joints, but the most common one is arthritis. By definition, arthritis is the inflammation (swelling) of one or more joints. There are many different types of arthritis, and your risk of developing most forms increases as you grow older. It’s estimated that 22.7% of American adults (54.4 million) have arthritis. Within those people, around 43.5% (23.7 million) are unable to fully perform their usual daily activities due to their arthritis. These activities include:
grasping small objects
reaching above the head
sitting or standing for around 2 hours
lifting or carrying up to 10 pounds
climbing stairs without having to rest
pushing or pulling heavy objects
walking a quarter of a mile
stooping, bending, or kneeling
Having limitations to these simple tasks can lead to physical inactivity, which is associated with many serious conditions like heart disease, diabetes, and obesity. Therefore, it’s important to take the necessary preventive measures as early as you can to identify and treat arthritis.
Bone health screening
The United States Preventive Services Task Force (USPSTF) recommends screening for osteoporosis to prevent fractures in all women who are 65 years and older, and postmenopausal women younger than 65 years old who are at increased risk of osteoporosis. Currently, there’s still not enough evidence to assess whether or not screening will be beneficial in men. Once every 24 months (or more if medically necessary), Medicare part B covers bone mass measurements if you meet certain conditions.
Bone density test
The USPSTF reviewed the accuracy of two bone density screening tests: DEXA (dual-energy x‑ray absorptiometry) and QUS (quantitative ultrasound).
DEXA is the most commonly used method in diagnosing osteoporosis. It uses radiation to measure the bone density of central bone sites like the hip and lower spine, which is the accepted standard in the diagnosis of osteoporosis. Peripheral bone sites like the heel or forearm can also be used to identify low bone mass, but central bone sites are more accurate in identifying the condition. The T‑score on your DEXA scan represents how your bone mass differs from the bone mass of a healthy 30-year-old adult. A T‑score between ‑1.0 and ‑2.5 means you have osteopenia, while a T‑score lower than ‑2.5 means you have osteoporosis. On the other hand, the Z‑score compares your bone density to the bone density of people that are your age and gender. It’s mostly used for children, young adults, premenopausal women, and men below 50 years old. In these cases, a low Z‑score may mean that there’s an underlying medical condition other than osteoporosis, or medications that are causing bone density to be lower than normal.
The QUS test estimates fracture risk at peripheral sites, and it’s been gaining popularity in medical settings because it does not involve the use of radiation. However, it mostly measures bone quality (structure, composition, and mass), and not bone density. This creates a barrier to its use since bone density measurement is the current diagnostic standard for osteoporosis.
Clinical risk assessment tools
Risk assessment tools such as ORAI (Osteoporosis Risk Assessment Instrument), OSIRIS (Osteoporosis Index of Risk), OST (Osteoporosis Self-assessment Tool), SCORE (Simple Calculated Osteoporosis Risk Estimation), and FRAX (Fracture Risk Assessment Tool) are questionnaires that can be used to help doctors determine if you need to be screened with bone density tests. These assessment tools provide moderate accuracy in identifying your risk of osteoporosis and osteoporotic fractures.
Calcium and Vitamin D levels
Although calcium and vitamin D play an important role in bone formation, it has been shown that taking supplements is not likely beneficial and may even be harmful. The recommended dietary allowance (RDA) of calcium is 1000 milligrams (mg) in men 51–70 years old, and 1200 mg in women above 50 years old and men over 70. The RDA for vitamin D is 15 micrograms (mcg) in those between 51–70 years old, and 20 mcg in those over 70 years old. Usually, these levels can be attained with diet alone, and exceeding these levels through intake of supplements may even have some risks. Because of this, screening of calcium and vitamin D levels for the diagnosis and prevention of osteoporosis is not routinely done.
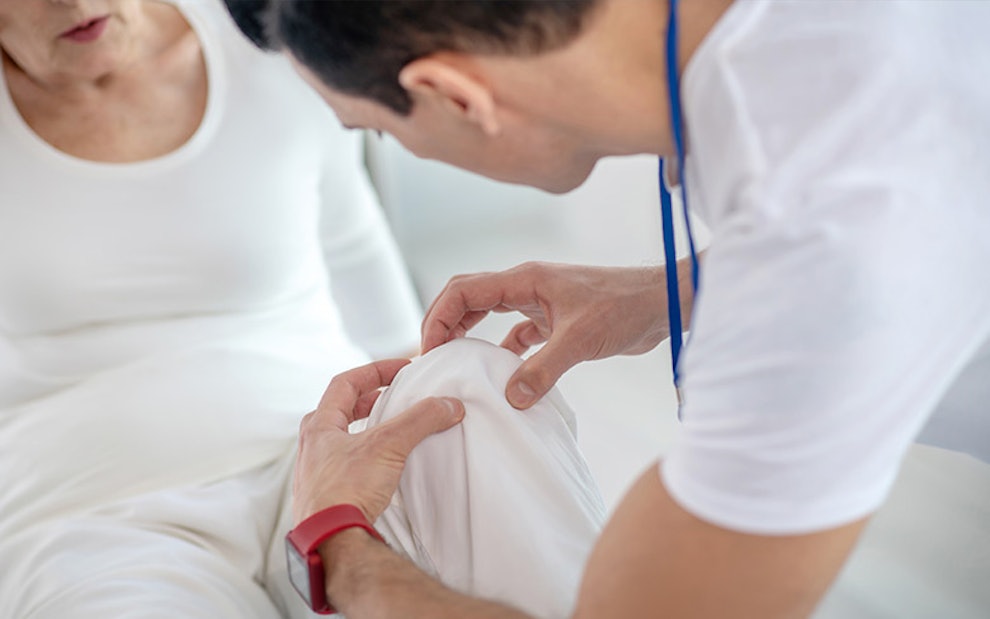
Joint health screening
Although arthritis is a common condition, there’s currently no standardized screening tool for it. Testing for arthritis is mostly used for diagnosing, treatment planning, and monitoring. But if you’re concerned that you may have arthritis, your doctor will be able to tell if you need to be tested. Usually, testing is recommended for those who are experiencing arthritis symptoms like pain, swelling, warmth, and redness in one or more joints. Tests for arthritis are usually non-specific, and diagnosis requires the combination of a person’s medical history, physical examination, and test results. For example, inflammation can be detected by measuring your white blood cell (WBC) count, erythrocyte sedimentation rate (ESR) or C‑reactive protein (CRP). But these levels can be elevated in a number of conditions, not just arthritis. Antinuclear antibody (ANA), cyclic citrullinated peptide (CCP) antibody, and rheumatoid factor (RF) may be present or elevated in autoimmune diseases like rheumatoid arthritis, but may be absent in other forms of arthritis.
Screening isn’t the only thing you can do to prevent your bones and joints from weakening. Exercising is one of the most important things you can do, along with maintaining a healthy diet. Physical activity makes your muscles strong which helps stabilize your joints and prevent them from wearing out, while eating a balanced diet ensures that you get the proper nutrients that your body needs, and helps manage your weight to prevent excess stress on your joints.
Bones and joints may weaken as you grow older, but there are a lot of things you can do to prevent this from happening, or at the very least slow it down. Awareness, timely screening, and appropriate lifestyle practices are key to avoiding the outcomes that may come with osteoporosis and arthritis, and it’s never too early to start practicing them.
Become a patient
Experience the Oak Street Health difference, and see what it’s like to be treated by a care team who are experts at caring for older adults.




