Article at a glance
CT scans are a common diagnostic test to detect many types of injuries or illnesses.
Medicare covers CT scans under Medicare Part B. However, what exactly Medicare pays will vary based on one’s specific health plan,
Medicare Part A will cover CT scans during hospital admission.

In the event a Medicare beneficiary needs diagnostic testing through a CT scan, they may be curious about how to prepare for the scan. Medicare patients may also be concerned about potential out-of-pocket costs associated with this computer imaging technique.
In most cases, Original Medicare will cover the majority of costs associated with receiving a CT scan. As well, Medigap policies or having a Medicare Advantage plan may help cut costs even more. That said, overall CT scan costs will vary based on the individual’s specific health care plan(s).
This article will explain everything Medicare beneficiaries need to know about how CT scans work under the federal Medicare program, including average costs and more.
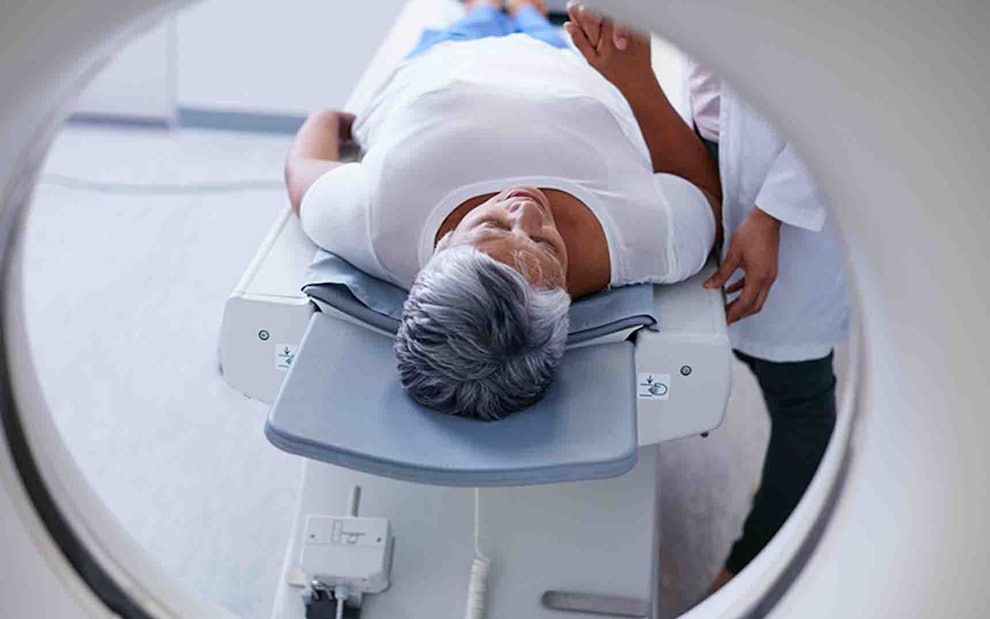
What Is A CT Scan?
A CT scan, also known as a CAT scan, is an imaging technique that uses computers and rotating X‑ray machines in order to create cross-sectional images of various internal body parts. CT stands for “computed tomography” or “computerized tomography”.
Why Are CT Scans Ordered?
A doctor orders this type of scan for suspected illness or injury. These scans can detect health issues in various parts of the body and helps doctors analyze the issue and how to treat it.
Parts of the Body CT Scans Read
CT scans can detect injuries or illnesses in various parts of the body such as:
Head
Shoulders
Spine
Heart
Abdomen
Knees
Chest
Does Medicare Cover CT Scans?
CT scans are considered to be one of several diagnostic non-laboratory tests covered by Medicare. These non-laboratory tests are covered under Medicare Part B, medical insurance. This includes MRI scans, EKGs, PET scans, and other diagnostic tests done in a doctor’s office or another outpatient setting such as an independent testing facility.
Criteria for CT Scan Coverage
That said, some criteria must be met in order for Medicare to cover a non-laboratory diagnostic test. Some such criteria include:
A healthcare provider who accepts Medicare has ordered the test
The test is performed at a Medicare-approved hospital or facility
Medical records indicate the test is medically necessary
As well, Medicare Part A, Medicare’s hospital insurance, may also provide CT scan coverage if the test is ordered during inpatient hospitalization.
What Is The Average Cost Of A CT Scan?
As a general rule, Medicare pays for 80 percent of the Medicare-approved amount for non-laboratory diagnostic tests. The patient is responsible for the remaining 20 percent. The total costs will depend on where the CT scan is performed, meaning whether it is performed on an inpatient or outpatient basis.
For example, CT scans done in ambulatory surgical centers cost Medicare beneficiaries around $8.00. In this case, Medicare Part A covers the test. For CT scans performed in a hospital outpatient setting, the cost averages around $16.00 for Medicare beneficiaries. In this case, Medicare Part B covers the test.
Other factors that may play a role in out-of-pocket cost includes where the Medicare beneficiary lives and whether the Medicare Part B deductible has been met.
Note: These Medicare coverage estimates are based on facility and doctor fees, but additional costs may be involved. Medicare beneficiaries should consult their doctor or insurance company to confirm coverage. This checklist of questions and considerations is a helpful resource.
Do Medicare Advantage Plans Cover CT Scans?
Medicare Advantage plans, also known as MA plans or Medicare Part C, are Medicare plans offered via private insurance companies. These insurance companies are Medicare-approved.
A Medicare Advantage plan has the same covered services as Original Medicare. MA plans also have additional benefits. This means that beneficiaries with an MA plan may have a lower CT scan cost. They will need to confirm coverage.
Note: Learn more about Medicare Advantage plans at this resource.
Do Other Medicare Supplement Insurance Plans Cover CT Scans?
Medicare supplement insurance plans, also known as MedSupp or Medigap, are supplemental insurance policies that “fill in the gaps” of Original Medicare. Since these plans are in addition to Original Medicare, beneficiaries should expect their Medicare plan to still cover 80 percent of CT scan costs, with their financial responsibility being 20 percent, unless they’ve already met their yearly deductible.
As well, Medigap policies may reduce out-of-pocket costs. However, this is all dependent on the specific plan and insurance company.
Note: Learn more about Medigap at this resource.
How Do Prescription Drugs Work With a CT Scan?
At times, prescription medications may be needed to undergo a CT scan. Under Medicare Part B, these medications are not covered. That said, Medicare Part D, which is Medicare’s prescription drug coverage, would cover it.
FAQ
What part of Medicare covers CT scans?
Medicare Part A, which is considered Medicare’s “hospital insurance,” covers CT scans if they are ordered during an inpatient stay, such as if a patient is admitted to a skilled nursing facility. Medicare Part B, which is considered Medicares “medical insurance,” covers CT scans if they are ordered as an outpatient procedure.
Become a patient
Experience the Oak Street Health difference, and see what it’s like to be treated by a care team who are experts at caring for older adults.



