Article at a glance
Chemotherapy is a type of cancer treatment using various types of cancer drugs to stop the proliferation of cancer cells.
Medicare covers chemotherapy. This is true for those who choose to enroll in a Medicare Advantage plan as well. However, not all services associated with this type of cancer care may be covered. As such, coverage for prescription drugs (Medicare Part D) is incredibly important.

Receiving a cancer diagnosis can be a frightening and stressful experience. From coordinating health insurance coverage and out-of-pocket costs to understanding what cancer treatments are best for a specific diagnosis, there are many factors to navigate.
The main focus should be first and foremost on health and becoming well. This is why Medicare beneficiaries should be educated on everything about their Medicare coverage. Knowing exactly what is covered by their health care plan helps make the unexpected news easier to manage.
This article will explain everything Medicare beneficiaries need to know about Medicare and chemotherapy, as well as brief details on Medicare coverage for other types of cancer treatment.
Does Medicare Cover Cancer Treatment?
There are various cancer treatment services that may be necessary, depending on a cancer patient’s diagnosis. For example, breast cancer may have different treatment approaches than lung cancer. Potential types of cancer treatment include immunotherapy, standard chemotherapy, radiation, surgery, and ongoing follow-up with oncology specialists.
Does Medicare Cover Cancer Screenings?
Medicare covers cancer screenings. Learn more about recommended health screenings at this resource.
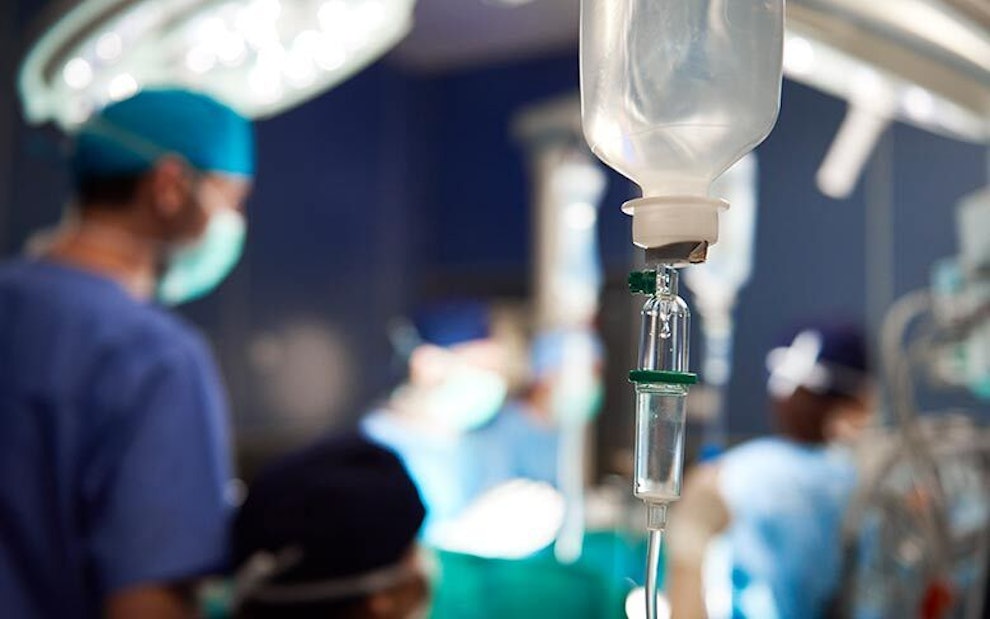
What Is Chemotherapy?
Chemotherapy is a type of cancer treatment that uses medication, known as chemotherapy drugs, to destroy cancer cells. These drugs prevent cancer cells from growing, dividing, and making more cells. Chemotherapy can be administered orally or intravenously (IV). There are various types of chemotherapy drugs that are used depending on the type of cancer and prognosis a patient has.
What Other Types Of Cancer Treatments Are Available?
There are various cancer treatment services that may be necessary, depending on a cancer patient’s diagnosis. For example, breast cancer may have different treatment approaches than lung cancer.
Does Medicare Cover Chemotherapy?
Medicare covers chemotherapy cancer treatment, both under Medicare Part A and Medicare Part B. Each Medicare Part is responsible for different portions of chemotherapy.
Medicare Part A
Medicare Part A is Medicare’s hospital insurance and covers chemotherapy within in-patient settings. Medicare Part A covers:
Inpatient hospital stays
Skilled nursing facility care
Home health care
Hospice care
Blood
Some clinical research study costs (must be in-patient)
Surgically-implanted breast prostheses following a mastectomy (surgery must have been in-patient)
Medicare Part B
Medicare Part B is medical insurance and covers outpatient services at a doctor’s office or freestanding clinic visit.
When it comes to chemotherapy treatments, Medicare Part B covers:
Doctor visits
Many intravenous chemotherapy drugs
Certain oral chemotherapy medication
Outpatient radiation therapy
Diagnostic tests
Durable medical equipment (wheelchairs, walkers, etc.)
Outpatient surgeries
Mental health services
Some preventive and screening services
Enteral nutrition equipment (feeding pump)
Some clinical research studies costs (must be outpatient)
Breast prostheses after a mastectomy (surgery must have been outpatient)
Note: A patient can still be considered outpatient, even if in the hospital due to their “observation status”. Medicare patients unaware of their classification should consult their healthcare provider.
Medicare doesn’t cover the following services:
Assisted living facilities room and board
Adult day care
Long-term nursing home care
Medical food or nutritional supplements (except enteral nutrition equipment)
Daily living services not requiring skilled care
Do Medicare Advantage Plans Cover Chemotherapy?
Medicare Advantage (MA) plans, or Medicare Part C, are essentially enhanced versions of Original Medicare. MA plans are provided through private insurance companies, bundling both Medicare Part A and B. As such, those with MA plans will receive the same level of coverage as those with Original Medicare.
Some MA plans may also include prescription drug coverage, known as Medicare Part D. However, not all MA plans include medication coverage. Medicare Advantage beneficiaries should always confirm what’s covered with their healthcare providers and/or their insurance company.
Does Medicare Supplement Insurance Cover Chemotherapy?
Medigap supplement insurance, also known as Medigap, fills in the gaps in Original Medicare coverage. This includes helping with payments for coinsurance, coinsurance, and deductibles. Learn more about Medigap at this resource.
Chemotherapy Costs
Copayments, coinsurance, and deductibles may apply for any of the aforementioned services. In general, a Medicare beneficiary usually pays a copayment for chemotherapy, which is covered under Part B, so long as it is within a hospital outpatient setting. For chemotherapy given in a doctor’s office or freestanding clinic, they pay 20% of the Medicare-Approved Amount. The Part B deductible also applies.
Do note, overall costs will vary and are dependent on:
Other insurance
How much a doctor charges
Whether the doctor accepts the assignment
Facility type
Location of the test, item, or service
A patient should always talk to their health care provider to confirm any out-of-pocket costs they will be responsible for.
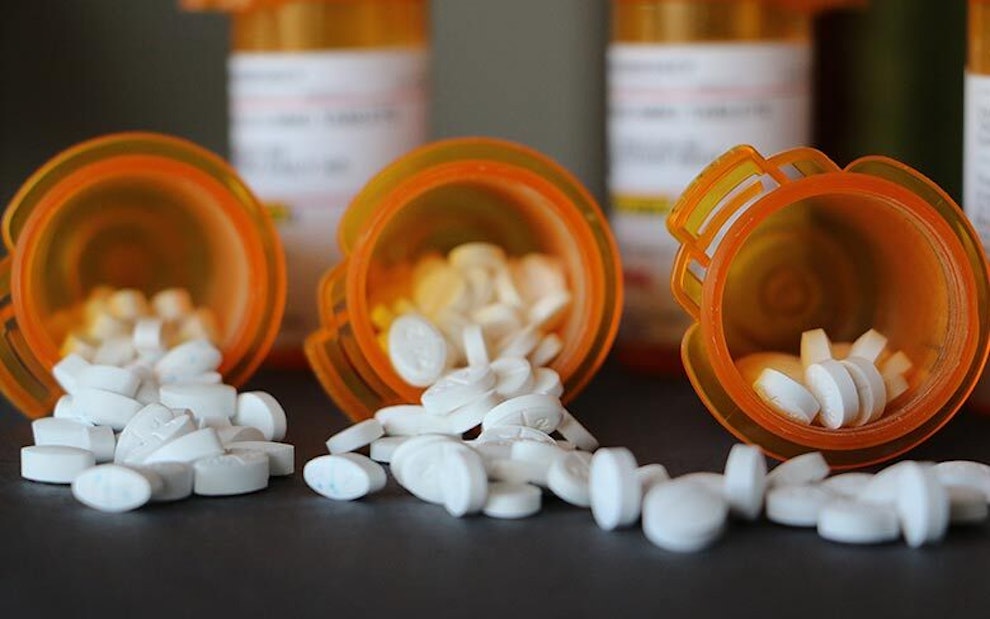
The Importance of Prescription Drug Coverage
In the event Medicare Part B does not cover the cancer drugs needed for chemotherapy, Medicare Part D may provide coverage. However, there are certain medications that may not be covered under Part D.
Because chemotherapy is an aggressive treatment, it can also hurt healthy cells in the process of destroying cancer cells. This healthy cell damage is what is associated with common side effects of chemotherapy, including nausea, fatigue, and headaches. As such, other medications may be necessary, such as anti-nausea drugs and pain medication.
Note: Medicare beneficiaries must be enrolled in Part D or have an MA plan that contains Part D. It is important to remember that Medicare beneficiaries are not automatically enrolled in a prescription drug plan.
Sources
- www.medicare.gov/coverage/chemotherapy
- www.medicare.gov/Pubs/pdf/11931-Cancer-Treatment-Services.pdf
- www.medicare.gov/drug-coverage-part‑d/how-to-get-prescription-drug-coverage
- www.cancer.net/navigating-cancer-care/how-cancer-treated/chemotherapy/understanding-chemotherapy
- www.cancer.net/navigating-cancer-care/how-cancer-treated/chemotherapy/side-effects-chemotherapy
- https://www.medicare.gov/supplements-other-insurance/whats-medicare-supplement-insurance-medigap
Become a patient
Experience the Oak Street Health difference, and see what it’s like to be treated by a care team who are experts at caring for older adults.



